TL;DR:
- Structured team therapy can improve workplace wellbeing and deliver measurable business returns.
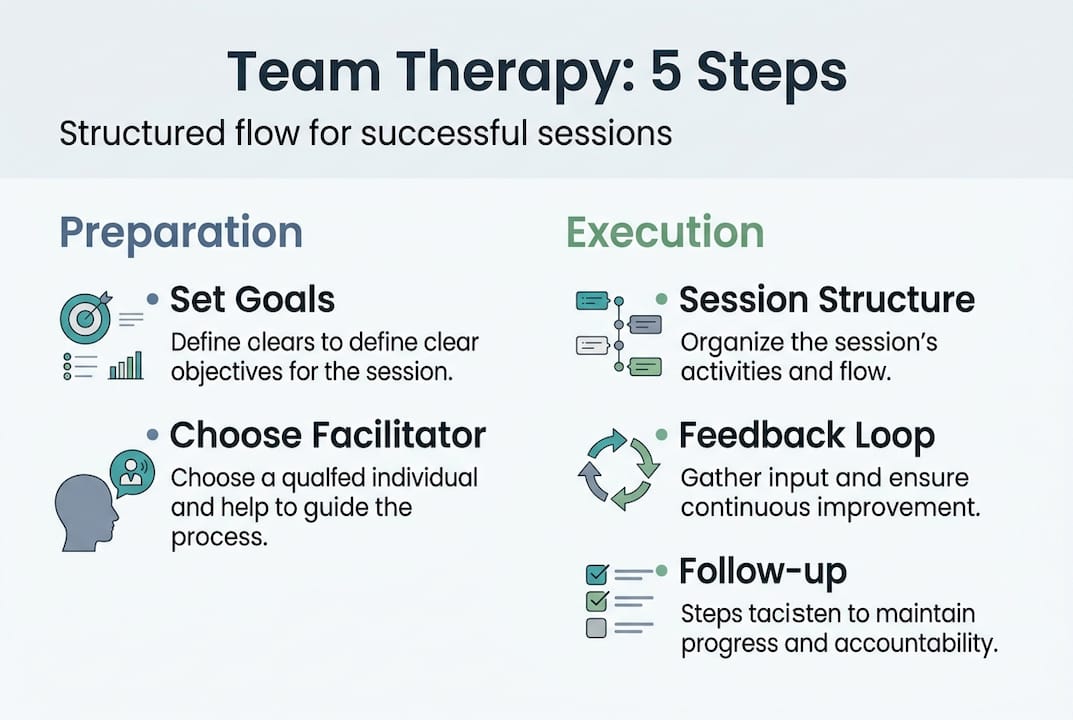
- Effective sessions require thorough preparation, participant screening, and skilled facilitation.
- Ongoing measurement and integrated follow-ups are essential for lasting team and individual improvements.
Unresolved conflict, rising stress levels, and persistent absenteeism quietly erode team performance before most leaders notice. Structured team therapy sessions offer a practical, evidence-based response. Group therapy matches individual therapy efficacy and can deliver measurable workplace returns, making it one of the most underused tools in corporate wellbeing. This guide walks you through every stage, from preparation and screening to running sessions, troubleshooting challenges, and measuring lasting impact, so your team gets the full benefit.
Table of Contents
- Preparing for a team therapy session
- Running the session: structure and methodologies
- Troubleshooting: common challenges and how to address them
- Measuring outcomes and ensuring lasting impact
- A fresh perspective: what most corporate teams miss about team therapy sessions
- Connect with GuideMe for tailored team therapy support
- Frequently asked questions
Key Takeaways
| Point | Details |
|---|---|
| Structured approach matters | Careful preparation and step-by-step session structure maximise psychological safety and engagement. |
| Blend methods for impact | Combining cognitive-behavioural, interpersonal, and psychoeducational models enhances workplace outcomes. |
| Troubleshoot proactively | Anticipate dropouts and conflicts using tailored protocols and ongoing monitoring. |
| Measure and reinforce | Use diagnostic tools and scheduled follow-ups to sustain positive team dynamics over time. |
Preparing for a team therapy session
With a clear understanding of the session's benefits, the next step is thorough preparation to ensure successful outcomes. Preparation is where most corporate teams either set themselves up for success or quietly undermine the process before it begins.
Participant screening is the foundation. Pre-group preparation and screening are essential, and high-risk participants should not be included without proper individual support in place first. Screening assesses psychological readiness, group fit, and any risk factors that could disrupt the session or harm participants. This is not about exclusion for its own sake. It is about protecting everyone in the room.
When assessing fit, consider the following criteria:
- Psychological readiness: Is the participant stable enough to engage in group reflection without becoming destabilised?
- Interpersonal risk: Does the individual have a history of behaviour that could undermine psychological safety for others?
- Motivation: Is the participant willing to engage, or are they attending under pressure?
- Exclusion indicators: Active crisis, severe untreated mental health conditions, or recent trauma requiring individual support first.
A structured diagnostic tool such as the Team Canvas helps map team dynamics and surface tension points before the session begins. Pairing this with pre-session screening gives facilitators a much clearer picture of where the group sits emotionally and relationally.
Choosing a licensed facilitator is equally critical. This is not a role for an HR generalist or a well-meaning manager. A qualified group therapist or organisational psychologist brings clinical judgement that protects participants and guides the group through difficult moments.
Comparison of common screening methods:
| Screening method | Best for | Key benefit |
|---|---|---|
| Team Canvas diagnostic | Mapping group dynamics | Surfaces relational tension early |
| Individual pre-session interview | Assessing personal readiness | Identifies high-risk participants |
| Standardised questionnaire | Scalable screening | Consistent, comparable data |
| Manager referral assessment | Flagging known concerns | Contextualises existing team issues |
Materials checklist before your session:
- Confidentiality agreements for all participants
- Room set-up in a circle or horseshoe arrangement to encourage dialogue
- Facilitator notes and session objectives printed in advance
- Feedback forms for post-session measurement
- Contact details for individual follow-up support if needed
Good collaboration practices begin before anyone enters the room. The preparation stage is where trust is either built or lost.
Pro Tip: Begin every preparation process by establishing psychological safety explicitly. Tell participants in writing, before the session, exactly what is and is not confidential. Ambiguity here destroys trust before the session even starts.
Running the session: structure and methodologies
With successful preparation, the practical running of the session becomes the next priority. A well-structured session does not happen by accident. It follows a deliberate sequence that creates safety, builds engagement, and closes with clear commitments.

Sessions typically last 60 to 120 minutes, structured around check-in, a main activity, and closing action planning. The optimal group size sits between seven and ten participants, large enough for diverse perspectives but small enough for genuine dialogue.
Typical session timetable:
| Phase | Duration | Purpose |
|---|---|---|
| Check-in and grounding | 10-15 minutes | Settle the group, establish safety |
| Psychoeducation or skill input | 15-20 minutes | Introduce the session's core theme |
| Main activity or group exercise | 30-45 minutes | Practice, reflection, and dialogue |
| Closing and action planning | 10-15 minutes | Commit to behavioural changes |
Step-by-step session structure:
- Opening ritual: Begin with a brief grounding exercise. This might be a one-word check-in or a short breathing practice. It signals the transition from work mode to reflective mode.
- Psychoeducation input: The facilitator introduces the session's theme, whether that is communication, conflict resolution, or stress management, using clear, accessible language.
- Main group activity: Use structured exercises such as the Johari Window to explore blind spots in team communication, or Personal Histories to build empathy across the group. Cognitive Behavioural Group Therapy (CBGT) techniques and Interpersonal Therapy (IPT) frameworks work well here.
- Closing action plan: Each participant names one specific behavioural commitment they will carry into the working week. This step is non-negotiable. Without it, insight stays in the room.
Review the session structure overview to understand how these phases connect across a multi-session programme. For broader clinical guidance, the group session guidelines provide a thorough reference point.
Safety note: Psychological safety is not a given. Microaggressions, dismissive language, or dominant voices can rupture trust quickly. Facilitators must actively monitor group dynamics and intervene early when safety is compromised. A session that feels unsafe will cause more harm than no session at all.
Troubleshooting: common challenges and how to address them
After setting up and running the session, it is vital to anticipate and manage common pitfalls. Even well-prepared sessions encounter obstacles. Knowing what to expect, and how to respond, makes the difference between a session that recovers and one that collapses.
Dropout rates in group therapy can reach 10 to 23%, and conflict repair protocols alongside add-on individual sessions significantly improve retention and outcomes. These figures are not a reason for alarm. They are a reason to plan.
Common challenges and response strategies:
- Participant dropout: Address this by revisiting the pre-session agreement and offering a brief individual check-in. Sometimes a participant simply needs reassurance before re-engaging.
- Microaggressions: Facilitators should name these directly but calmly in the moment. Ignoring them signals that harmful behaviour is acceptable. Refer to affirming group experiences guidelines for structured repair protocols.
- Interpersonal conflict: Use structured dialogue techniques to give each party space. Avoid taking sides. The facilitator's role is to hold the space, not adjudicate.
- Disengagement: If participants are visibly withdrawn, introduce a low-stakes paired activity to rebuild connection before returning to the main exercise.
- Edge cases: For participants who present with heightened distress during a session, have a clear protocol for stepping outside with a designated support person. Safety always comes first.
Routine Outcome Monitoring (ROM) is a practical tool here. Short pulse surveys completed by participants during and after sessions give facilitators real-time data on engagement and safety. This is far more reliable than reading the room alone.
Review participant fit preparation to ensure your screening process reduces these risks from the outset.
Pro Tip: Send a two-question pulse survey immediately after each session. Ask participants to rate their sense of safety and their level of engagement on a simple scale. Patterns across sessions will show you exactly where to focus your troubleshooting efforts.
Measuring outcomes and ensuring lasting impact
Once challenges are managed, measuring and reinforcing outcomes underpins ongoing team improvement. A single session, however well run, rarely produces lasting change on its own. What sustains impact is a structured follow-up process tied to clear measurement.
Post-session measurement process:
- Immediate feedback: Collect session feedback forms within 24 hours while experience is fresh.
- One-month booster: A shorter follow-up session revisits commitments made in the closing action plan and addresses any emerging tension.
- Three-month review: Use the CORE-R assessment tool to measure changes in psychological wellbeing and team functioning since the initial session.
- Six-month pulse survey: A brief team-wide survey captures sustained behavioural change and flags any regression.
- Ongoing measurement: Integrate session effectiveness metrics into your broader HR reporting to track trends over time.
The CORE-R is a validated clinical tool that measures outcomes across four domains: subjective wellbeing, problems and symptoms, life functioning, and risk. It provides a reliable baseline and a comparable follow-up measure. Combined with a team health assessment framework, it gives HR leaders both clinical and organisational data in one picture.
The ROI case is compelling. Team therapy can achieve ROI up to 2.3x in workplace behavioural health programmes, with net savings of $159 per member per month. These are not marginal gains. They represent a genuine business case for sustained investment.
Behavioural commitments made in session need reinforcement. Encourage team leaders to reference session themes in regular one-to-ones and team meetings. This keeps the work alive between formal sessions and signals that the organisation takes it seriously.
A fresh perspective: what most corporate teams miss about team therapy sessions
Beyond the practical steps, there is something most teams consistently overlook. They treat team therapy as an event rather than a process. One session gets booked, delivered, and ticked off. Then nothing changes, and leadership wonders why.
Real change requires ongoing structure. Hybrid models combining group and individual add-on sessions consistently outperform group-only approaches because they address both collective and personal dimensions of the work. A participant may engage well in the group but carry something unresolved that only surfaces in individual support.
Early structure also matters more than most teams realise. Cohesion and engagement are predicted by how clearly the process is set up from the beginning, not by how skilled the facilitator is in the room. Rushing past the preparation stage to get to the "real work" is the most common mistake we see.
Start with psychological safety, not skills. Teams that begin with trust-building exercises before introducing any therapeutic content show stronger disclosure, deeper engagement, and better retention. Skills can be taught at any point. Trust takes time, and it cannot be shortcut.
Connect with GuideMe for tailored team therapy support
To implement these strategies with confidence, professional support can make all the difference.
GuideMe understands that navigating team therapy can feel complex, especially when you are balancing clinical rigour with the realities of a busy workplace. Our platform combines human expertise with AI-powered matching to connect your team with the right therapist from the very beginning.
Whether you are planning your first structured session or looking to build a sustained programme, our corporate team therapy solutions are designed to support every stage of the process. From pre-session screening to follow-up measurement, GuideMe helps your team access the right support with clarity and confidence.
Frequently asked questions
What is the ideal group size for corporate team therapy sessions?
The optimal group size is 7 to 10 participants, which balances diverse perspectives with enough intimacy for genuine dialogue and engagement.
How long should each team therapy session last?
Sessions typically last between 60 and 120 minutes, providing sufficient time for a structured check-in, the main activity, and a meaningful closing action plan.
How are participants screened for suitability?
Screening involves assessing psychological fit, risk factors, and readiness for group dynamics, typically using diagnostics such as the Team Canvas alongside individual pre-session interviews.
What challenges can arise during sessions?
Common issues include dropouts, conflicts, disengagement, and microaggressions. Structured repair protocols and add-on individual sessions are the most effective tools for managing these challenges.
How is progress measured after a session?
Progress is tracked using validated tools like CORE-R and pulse surveys, with follow-up boosters scheduled at one, three, and six months to sustain and measure lasting behavioural change.
